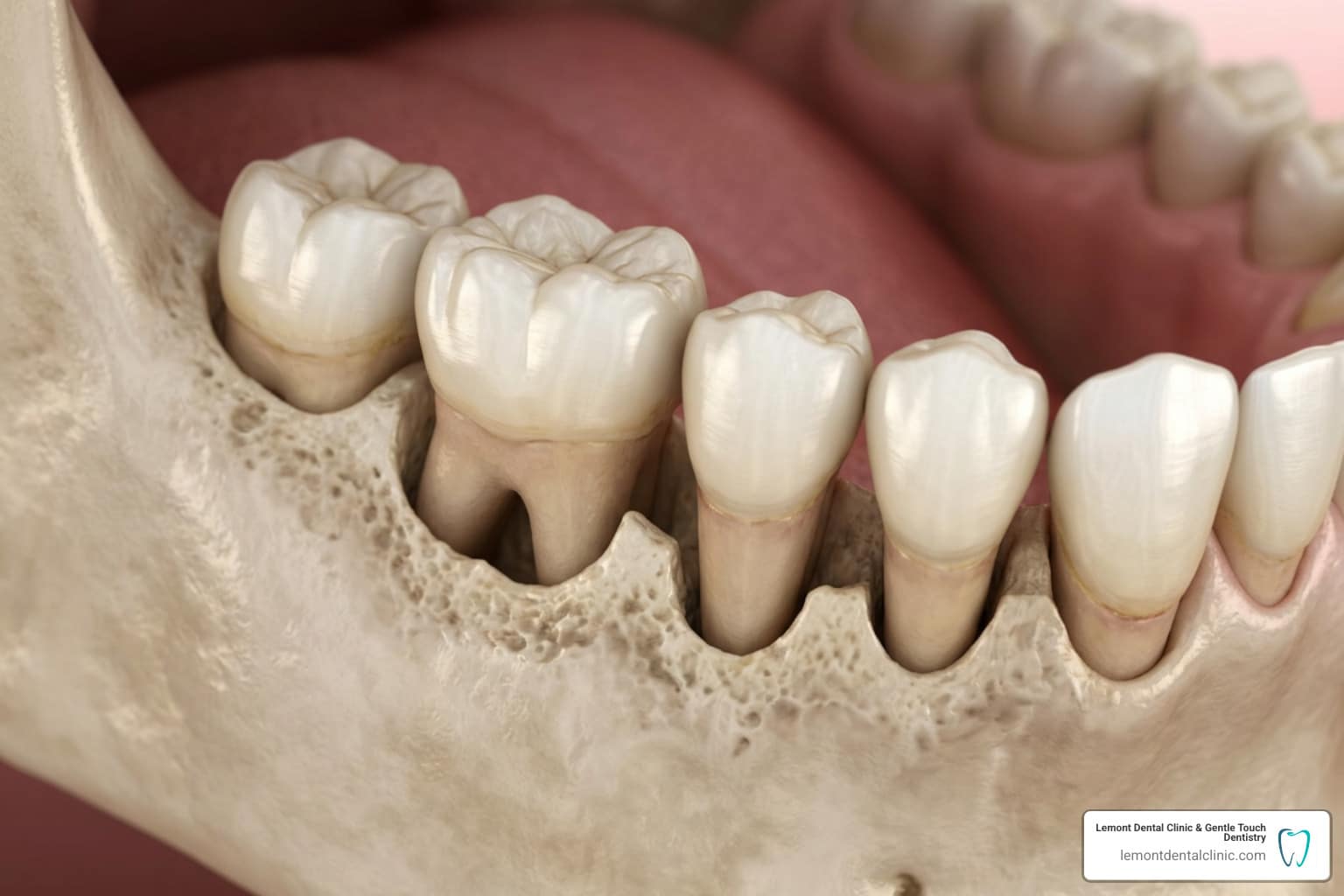
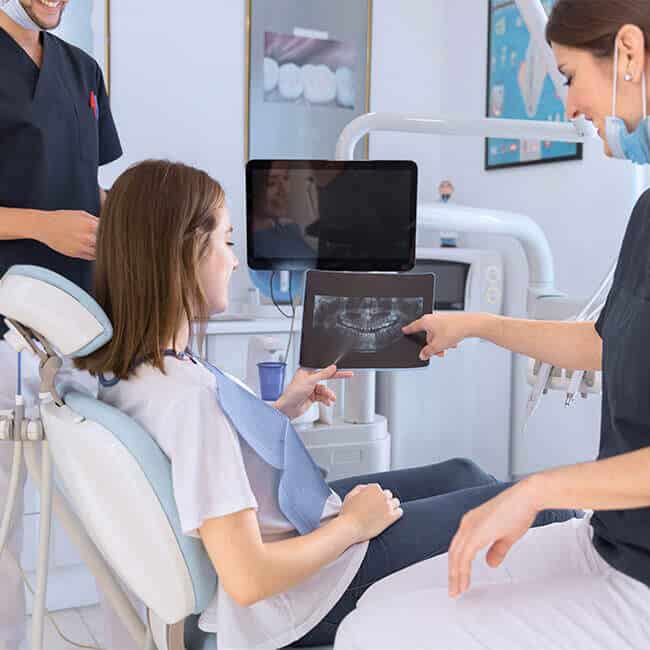
The Silent Threat You Can’t Feel Until It’s Serious
Teeth bone loss is the gradual breakdown of the jawbone that holds your teeth in place — and most people don’t know it’s happening until real damage is done.
Here’s a quick summary of what you need to know:
- What it is: Loss of bone density and volume in the jaw, usually around the teeth
- Main causes: Gum disease (periodontitis), missing teeth, smoking, teeth grinding, and osteoporosis
- Early signs: Receding gums, loose teeth, shifting bite, persistent bad breath
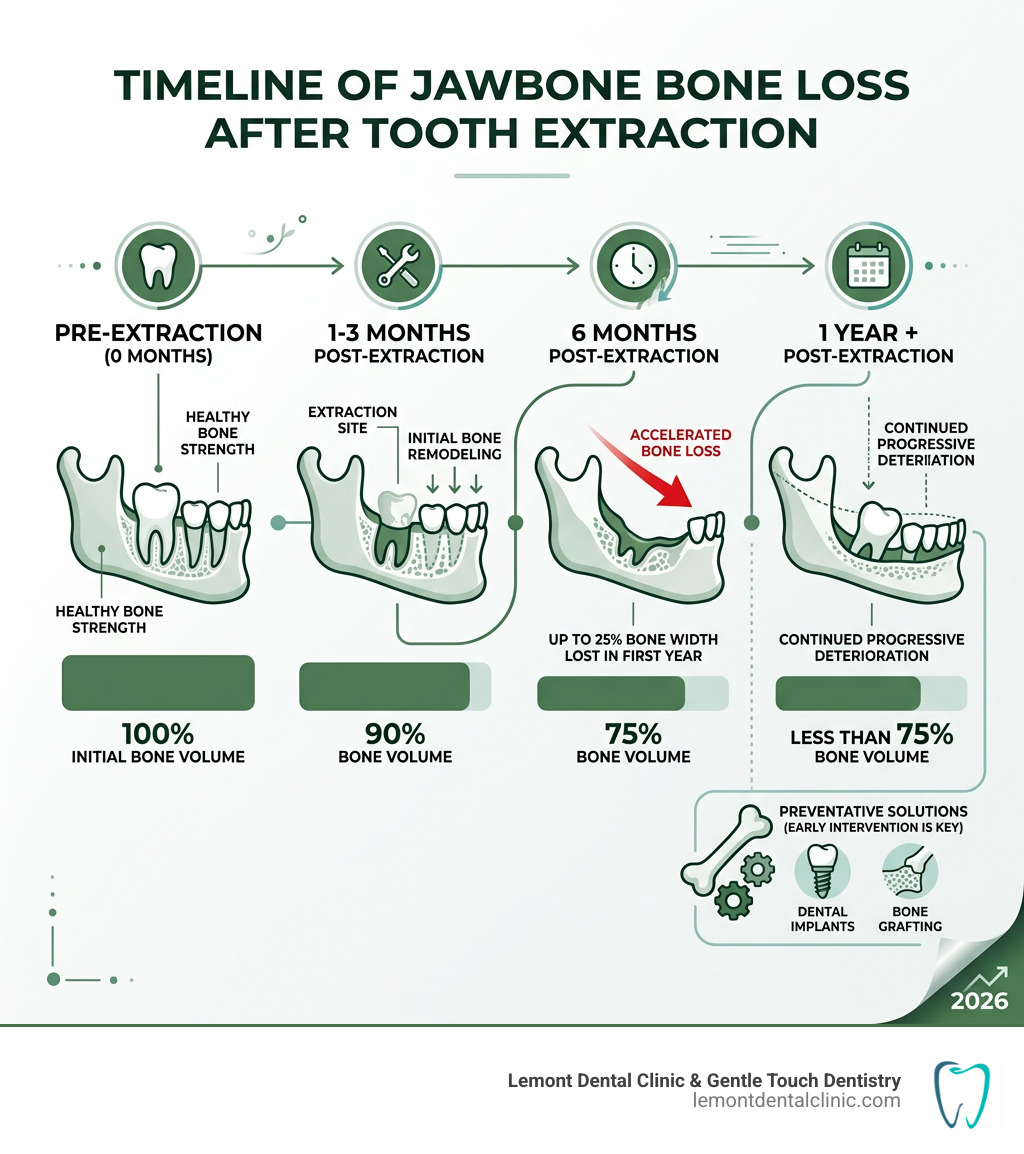
- How fast it progresses: Up to 25% of jawbone width can disappear within the first year after a tooth is lost
- Can it be treated? Yes — early stages can be halted; advanced cases can be rebuilt with procedures like bone grafting or dental implants
This condition is often called a “silent threat” for a reason. It causes little to no pain in its early stages, so it quietly progresses beneath the surface — sometimes for months or years — before you notice anything wrong.
By the time most people seek help, significant bone volume has already been lost. That loss doesn’t just affect your teeth. It can change the shape of your face, make dental restorations harder, and impact your overall health.
The good news? Knowing what to look for — and acting early — makes a huge difference.
Teeth bone loss vocabulary:
Understanding the Causes of Teeth Bone Loss
At Lemont Dental Clinic & Gentle Touch Dentistry, we often see patients who are surprised to learn that their jawbone is shrinking. The jawbone, specifically the alveolar bone, is a “use it or lose it” type of tissue. It requires constant stimulation to stay healthy. When that stimulation is gone, or when infection sets in, the bone begins to dissolve.
Periodontal Disease: The Leading Culprit
The most common cause of teeth bone loss is Periodontal Disease: The Sneaky Enemy of Teeth. It starts with bacterial plaque—that sticky film that forms on your teeth. If not removed, it hardens into tartar (calculus). Bacteria in tartar release toxins that trigger an inflammatory response. Your body’s own immune system, in an attempt to fight the infection, begins to break down the connective tissue and bone that hold your teeth in place.
Tooth Extraction and Missing Teeth
When a tooth is removed and not replaced, the underlying bone no longer receives the “chewing pressure” it needs. Without this mechanical stimulus, the body decides the bone is no longer necessary and begins to resorb it. This is why having a missing tooth for years can lead to a collapsed facial appearance.
Health and Lifestyle Factors
Several other factors can accelerate this process:
- Smoking: Tobacco use disrupts the blood supply to the gums and interferes with the function of gum cells, making bone loss occur much faster.
- Osteoporosis: This systemic condition leads to decreased bone density throughout the body, including the jaw. Research shows that women with osteoporosis often experience higher rates of tooth loss.
- Bruxism (Teeth Grinding): Constant, heavy pressure from grinding can stress the supporting structures, leading to bone recession.
- Facial Trauma: A forceful blow to the jaw can damage the bone or knock out teeth, stopping the stimulation needed for bone maintenance.
| Cause |
Severity |
Primary Mechanism |
| Periodontitis |
High |
Bacterial infection & inflammatory response |
| Tooth Extraction |
High |
Lack of mechanical stimulation (chewing) |
| Smoking |
Moderate/High |
Reduced blood flow & impaired healing |
| Osteoporosis |
Moderate |
Systemic reduction in bone mineral density |
| Bruxism |
Low/Moderate |
Excessive occlusal (bite) force |
The Biological Process: How Bone Resorption Occurs
To understand teeth bone loss, we have to look at the “construction crew” inside your mouth. Your bones are living tissues that are constantly being remodeled by two types of cells:
- Osteoblasts: These are the “builders” that lay down new bone tissue.
- Osteoclasts: These are the “demolition crew” that break down old or unnecessary bone.
In a healthy jaw, these two work in perfect balance. However, when a tooth is lost or infection is present, the balance shifts. Scientific research on osteoclast activation shows that inflammatory markers and a lack of physical stress (chewing) signal the osteoclasts to go into overdrive.
The alveolar ridge—the part of the jawbone that contains the tooth sockets—is particularly sensitive. Statistics show that up to 25% of the bone width in that area can be lost within just the first 12 months after an extraction. This resorption continues gradually throughout life unless an intervention, like an implant, is made.

Recognizing the Early Signs and Symptoms
Because teeth bone loss is a “silent threat,” you need to be a bit of a detective. You won’t feel your bone dissolving, but you will see the effects on the structures around it.
- Loose or Shifting Teeth: If your teeth feel “wiggly” or you notice new gaps forming between them, the bone support is likely failing.
- Receding Gums: As the bone beneath the gums shrinks, the gum tissue follows suit, making the teeth look longer and exposing the sensitive roots.
- Persistent Bad Breath: This is often a sign of deep periodontal pockets where bacteria are actively destroying bone.
- Changes in Facial Shape: Significant bone loss can lead to a “sunken” look around the mouth. The distance between the nose and chin may decrease, leading to premature wrinkles and a collapsed facial profile.
- Difficulty Chewing or Jaw Pain: As the bite shifts due to moving teeth, you may experience discomfort in the jaw joints (TMJ).
If we suspect you are experiencing teeth bone loss at our Lemont or Palos Hills offices, we use advanced technology to see what’s happening beneath the surface. You can learn more about our foundational care on our General Dentistry Services page.
- Digital X-rays: These provide a 2D view of the bone levels around each tooth, allowing us to spot “pockets” of bone loss.
- CBCT 3D Scans: This is the gold standard for modern dentistry. A Cone Beam Computed Tomography scan creates a 3D map of your jaw, showing us the exact height, width, and density of your bone. This is crucial for planning dental implants.
- Periodontal Probing: We use a tiny instrument to measure the depth of the space between your teeth and gums. Deep “pockets” (usually over 3mm) indicate that bone loss is occurring.
Treatment Options: Reversing and Managing Bone Loss
While we can’t always “grow back” bone naturally, modern restorative dentistry offers incredible ways to rebuild what was lost.
- Bone Grafting: This involves placing bone graft materials (which can be your own bone, processed donor tissue, or synthetic materials) into the area of loss. This graft acts as a scaffold, encouraging your body to deposit new, natural bone.
- Socket Preservation: We perform this at the time of extraction. By filling the empty socket with graft material immediately, we can significantly reduce the amount of bone that shrinks away during healing.
- Sinus Lift: If you have bone loss in the upper back jaw, your sinuses might be too close to the area where an implant needs to go. A sinus lift gently moves the sinus membrane upward and places bone graft underneath to create a solid foundation.
- Deep Cleaning (Scaling and Root Planing): For bone loss caused by gum disease, a Deep Cleaning is the first step. We remove the tartar and bacteria from deep beneath the gum line to stop the infection and allow the tissues to heal.
Preventing Teeth Bone Loss Through Lifestyle Changes
Prevention is always more affordable and less invasive than surgery. We recommend these steps to keep your jaw strong:
- Flawless Hygiene: Brushing twice a day and flossing daily is non-negotiable. It keeps the bacterial “construction crew” from starting their demolition.
- Nutrition: Ensure you have adequate calcium and Vitamin D intake to support overall bone density.
- Quit Tobacco: If you smoke, quitting is the single best thing you can do for your oral health.
- Nightguards: If you wake up with a sore jaw, you might be grinding your teeth. A custom nightguard protects your teeth and bone from excessive force.
Explore all Our Services to see how we can help you maintain a healthy smile.
The Role of Implants in Stopping Teeth Bone Loss
If you have already lost a tooth, Dental Implants are the absolute best way to stop the “silent threat” of bone resorption. Unlike bridges or dentures that sit on top of the gums, an implant is a titanium post that is surgically placed into the jawbone.
Through a process called osseointegration, the bone actually fuses to the titanium. Because the implant acts like a natural tooth root, it provides the necessary stimulation to the jawbone every time you chew. This tells your body that the bone is still needed, effectively halting the resorption process. For those who qualify, we even offer Same Day Dental Implants to get you back to smiling immediately.
Frequently Asked Questions about Jawbone Health
Can dental bone loss be reversed without surgery?
In the very early stages, such as gingivitis, the inflammatory process can be reversed through professional cleanings and improved home care. However, once the physical bone tissue has dissolved (true periodontitis), it cannot “regrow” on its own. Rebuilding that lost volume typically requires regenerative procedures like bone grafting.
How fast does bone loss occur after losing a tooth?
It happens faster than most people realize. The most significant changes occur within the first 3 to 6 months. By the end of the first year, you can lose up to 25% of the bone width in that area. This is why we recommend discussing tooth replacement options before the extraction happens.
Is dental bone loss hereditary?
Genetics can play a role in how your body responds to bacteria or your natural bone density. However, lifestyle factors—especially oral hygiene, smoking, and regular dental visits—are much more influential. Even if your parents had “bad teeth,” you can maintain a strong jawbone with proactive care.
Conclusion
Teeth bone loss doesn’t have to be the end of your smile. At Lemont Dental Clinic & Gentle Touch Dentistry, we are dedicated to helping our neighbors in Lemont, Palos Hills, Oak Lawn, and the surrounding Chicago suburbs protect their oral health.
Whether you are concerned about receding gums, a missing tooth, or just want to ensure your jaw stays strong, our team uses the latest technology and experienced techniques to provide high-quality, affordable care. Don’t wait for the “silent threat” to become a loud problem. Schedule a consultation for Dental Implants today and let us help you keep your smile on a solid foundation.