What Is a Denture Base Material — and Why Does It Matter?
Denture base material is the foundation of any removable denture — the part that sits directly on your gum tissue, holds the artificial teeth in place, and distributes bite forces across your jaw.
Here’s a quick look at the most common types used today:
| Material Type |
Key Feature |
Best For |
| Heat-cured PMMA |
High strength (92.84 MPa) |
Full/partial dentures |
| Self-cured (cold-cure) PMMA |
Easy chairside use |
Repairs, relines |
| Microwave-cured PMMA |
Highest flexural strength (109.63 MPa) |
Lab fabrication |
| Thermoplastics (e.g., nylon) |
Flexible, monomer-free |
Allergy-sensitive patients |
| Cobalt-chromium alloy |
Rigid, durable metal framework |
Partial dentures |
| PEEK |
Lightweight, high-performance |
Advanced restorations |
Not all dentures are built the same. The material used for the base directly affects how long your denture lasts, how comfortable it feels, and even how safe it is for your body over time.
Most people think of dentures as one simple appliance. In reality, they’re a carefully engineered combination of materials — each chosen for specific mechanical, biological, and esthetic reasons.
Getting that combination right is what separates a denture that feels natural from one that causes discomfort, breaks too early, or triggers a reaction.
The most widely used option — polymethyl methacrylate (PMMA) — has dominated denture fabrication since the 1940s, when it replaced vulcanized rubber as the standard. By 1946, roughly 95% of all dentures were made using PMMA. Yet even today, no single material checks every box perfectly.
I’m Piotr Dederowski, and at Lemont Dental Clinic & Gentle Touch Dentistry, I work with patients every day who need restorative solutions — including dentures — built on the right denture base material for their specific needs. Understanding what goes into that base is the first step toward making a confident, informed decision about your dental care.
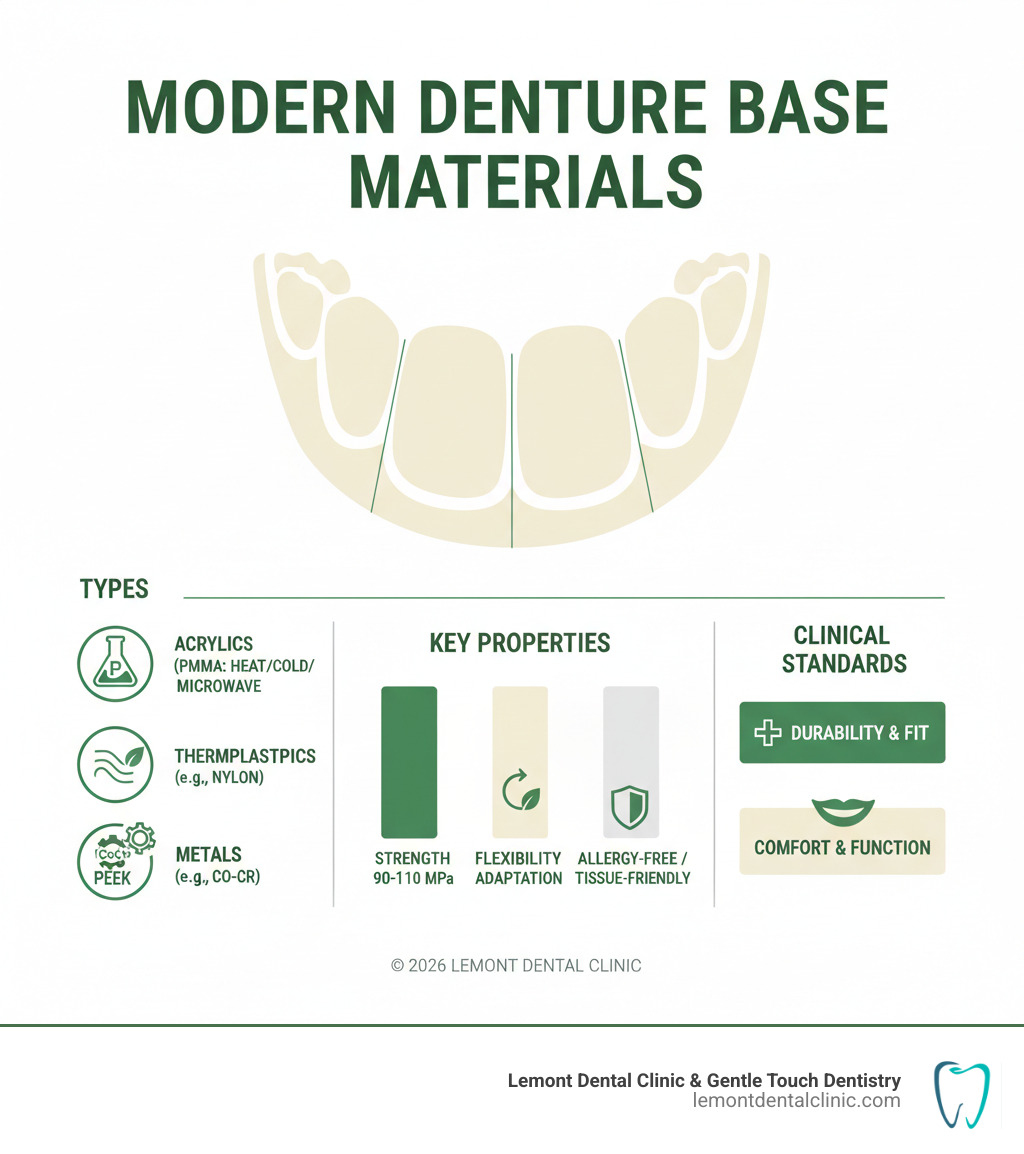
Related content about Denture base material:
The Evolution of Denture Base Material
The quest for the perfect denture base material is nearly as old as dentistry itself. Long before modern polymers, our ancestors used natural substances to replace missing teeth. Early attempts included carved wood, bone, and even ivory from hippos or walruses. While these looked somewhat like teeth, they were incredibly porous, absorbed odors, and deteriorated rapidly in the moist environment of the mouth.
In the mid-1800s, the “Vulcanite era” revolutionized the field. Vulcanite was a hard, chemically cured rubber that was relatively inexpensive and durable. However, it had a major drawback: it was opaque and dark, making it impossible to mimic the natural pink of healthy gums. Researchers also experimented with celluloid, but its popularity faded because it absorbed stains and left patients with a lingering taste of camphor.
The real breakthrough came in 1937 when Walter Wright introduced polymethyl methacrylate (PMMA). This transparent, stable, and easily pigmented resin allowed dentists to create Natural Looking Dentures for the first time. According to Scientific research on PMMA in prosthodontics, PMMA became the gold standard because it was easy to process and repair.
Today, we have moved into the era of thermoset resins and high-performance polymers like PEEK (polyetheretherketone) and light-cured resins. These modern materials allow for Implant Dentures and other advanced prosthetics that provide a level of comfort and function our ancestors could only dream of.
Essential Properties of a High-Quality Denture Base Material
When we evaluate a denture base material at Lemont Dental Clinic & Gentle Touch Dentistry, we look for a specific set of characteristics. A base isn’t just a holder for teeth; it must withstand the immense pressure of chewing while remaining gentle on the soft tissues.

The “ideal” material should possess high flexural strength to prevent snapping and high impact resistance so it doesn’t shatter if dropped during cleaning. It also needs good thermal conductivity—if you can’t feel the temperature of your coffee, it can lead to accidental throat burns.
To ensure patient safety, all materials should meet ISO 20795-1 standards. These standards regulate how much water the material absorbs (sorption) and how much of its chemical components leach out (solubility).
Mechanical Requirements for Denture Base Material
Mechanical integrity is non-negotiable. To prevent the denture from flexing and breaking under the stress of a steak dinner, the flexural strength must be greater than 50 MPa.
- Heat-cured PMMA: Traditionally offers a flexural strength of approximately 92.84 ± 4.73 MPa.
- Microwave-cured PMMA: Often reaches a higher strength of 109.63 ± 5.31 MPa.
- Fracture Toughness: This measures a material’s resistance to crack propagation. Heat-cured resins typically score around 2.06 MN/m^{3/2}, while cold-cured variants are slightly lower at 1.63 MN/m^{3/2}.
| Property |
Heat-Cured Resin |
Cold-Cured (Self-Cured) |
| Flexural Strength |
~92.84 MPa |
~84.40 MPa |
| Fracture Toughness |
2.06 MN/m^{3/2} |
1.63 MN/m^{3/2} |
| Residual Monomer |
0.2% – 0.5% |
3% – 5% |
Esthetic and Biological Standards for Denture Base Material
A denture shouldn’t look like a “piece of plastic.” We aim for high esthetic standards, including color stability (so it doesn’t turn yellow over time) and translucency (so natural gum color can peek through).
Biologically, the material must be non-toxic and non-irritating. ISO standards dictate that water sorption must be less than 32 µg/mm³ and solubility less than 1.6 µg/mm³. If these levels are too high, the denture can become a breeding ground for bacteria or cause Fixing Loose Dentures issues due to dimensional changes.
Classification and Types of Prosthetic Bases
Understanding the different classifications helps us tailor the prosthetic to your lifestyle. Most denture base material options fall into two categories: polymeric (plastics) and metallic.
Polymeric Options
- PMMA Variants: The most common choice. It can be modified with high-impact rubbers or reinforced with fibers to make it more durable for patients who might struggle with handling.
- Thermoplastics: These include materials like nylon or acetal resins. They are often used for flexible partial dentures because they don’t require metal clasps and are excellent for patients with monomer allergies.
- PEEK: A high-performance polymer used in aerospace and medicine, now making waves in dentistry for its light weight and “bone-like” elasticity.
- Cobalt-Chromium (Co-Cr): Often used for the framework of partial dentures. It is incredibly thin yet strong, allowing for better speech and taste.
- Gold Alloys and Titanium: Used for patients with specific metal sensitivities or those desiring premium durability.
According to Research on modified denture resins, adding nanofillers like silver or titanium oxide to these polymers can even provide antimicrobial properties, helping to prevent “denture breath” and fungal infections.
Processing Methods for Denture Base Material
How a material is processed changes its final performance:
- Heat-cured: The most common lab method, using a water bath or dry heat to trigger polymerization.
- Self-cured (Cold-cure): Uses a chemical activator. It’s faster but often leaves more residual monomer, which can irritate tissues.
- Light-cured: Uses visible blue light. Great for quick repairs.
- Injection Molding: Helps minimize “shrinkage,” ensuring a much more Snap-on Dentures style precision fit.
Advanced Fabrication and Digital Dentistry
We live in an era where “digital” isn’t just a buzzword—it’s a way to get a better-fitting denture. Digital dentistry uses CAD/CAM (Computer-Aided Design and Manufacturing) and 3D printing to create prosthetics with unmatched accuracy.
Traditional methods involve “packing and pressing” dough into a mold, which can lead to polymerization shrinkage of about 5-6%. Digital workflows, however, use pre-polymerized pucks or high-precision resins that virtually eliminate this shrinkage.
For the dental team, this means significant time savings. For example, high-impact pourable acrylics (HIPA) can deliver a 21% savings in hands-on working time compared to traditional heat-cure techniques. This efficiency allows us to focus more on the patient and less on the lab bench. You can find More info about restorative selection regarding the latest materials available to modern clinics.
Biocompatibility and Clinical Considerations
One of the biggest concerns with any denture base material is how it interacts with your body. The most common issue is the release of residual monomers—specifically methyl methacrylate (MMA).
In heat-activated resins, residual monomer levels are low (0.2% to 0.5%). However, in chemically activated (self-cured) resins, these levels can jump to 3% or 5%. If these monomers leach out, they can cause “allergic stomatitis,” a painful inflammation of the mouth lining.
To combat this, Scientific study on residual monomer levels suggests that soaking a new denture in water for 24-48 hours before the first wear can significantly reduce initial monomer release.
Modern Enhancements
We are also seeing incredible advancements in “smart” materials:
- Silver Nanoparticles: Incorporated into the base to kill bacteria and fungi like Candida albicans.
- Nanofillers: Such as Zirconia or Alumina, which increase the hardness and wear resistance of the base.
- Antimicrobial Agents: Help prevent the buildup of plaque on the denture surface.
These innovations aren’t just about making the denture last longer; they’re about keeping your mouth healthy. If you’re curious about the process, you might want to read about What Happens During a Denture Reline? to see how we maintain these materials over time.
Frequently Asked Questions about Denture Materials
What is the most common material used for denture bases?
Polymethyl methacrylate (PMMA) remains the most widely used material. It is favored for its ease of processing, excellent esthetics, and the ability to be easily repaired if it breaks.
How does 3D printing compare to traditional heat-curing?
3D printing offers a faster turnaround and a more precise fit because it bypasses many of the manual steps where errors can occur. However, traditional heat-cured resins still currently hold a slight edge in terms of overall long-term impact strength in some clinical studies.
“Better” depends on your needs. Metal bases (like Cobalt-Chromium) are much stronger and can be made thinner, which many patients find more comfortable for speech. However, they are more difficult to adjust and more expensive than standard acrylic.
Conclusion
Choosing the right denture base material is a collaborative process between you and your dental team. At Lemont Dental Clinic & Gentle Touch Dentistry, we pride ourselves on staying at the forefront of restorative technology to ensure our neighbors in Lemont and Palos Hills receive the best possible care.
Whether you need a simple partial or a complex set of Implant Dentures, our goal is to provide a solution that is durable, beautiful, and biocompatible. We understand that your smile is an investment, and we are here to help you protect it with quality materials and expert craftsmanship.
If you’re ready to explore your options, we invite you to check out our Welcome Promotion and schedule a consultation at a location near you.
For more information on finding the right fit, visit our Dentures Near Me page. We look forward to helping you smile with confidence again!